Today’s high-tech patient simulators help grow student skills and health care workforce
At Central Maine Community College in Auburn, a high-tech mannequin named Victoria is pregnant with her baby, Tory.
Also referred to as a simulator, Victoria can go into labor and deliver the baby. Both mannequins have realistic blood pressure, pulses, bowel sounds and eyes that blink. They can be made to seem like they’re speaking.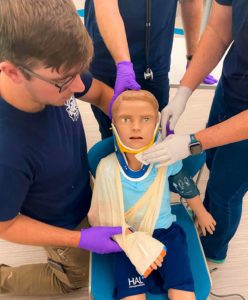
“We control the rate of labor, we have the contractions on one screen and we’ll have the fetal heart rate on another screen,” says Kathy McManus, chair of the college’s nursing program. “Students can look at how mom is doing, how baby is doing in utero – and the advantage is that we can stop and start. Those are teachable moments.”
Simulators and other high-tech equipment used to train students in the health care professions are getting more sophisticated all the time.
And simulation capacity is expanding. For example, new simulation technology and simulation coordinator positions are among key elements as Maine’s community college system looks to double its nursing program to 480 students per year, thanks to a $2.5 million allocation included in Maine’s supplemental budget earlier this year and matched by MaineHealth and Northern Light Health.
The expansion is part of an ongoing effort to use simulated environments to provide near-real-world experiences to students in supervised training settings, says Jessica Dreves, chair of the nursing department at Southern Maine Community College in South Portland.
Leading institutions use advanced simulation technology to improve graduates’ competence, especially in clinically high-risk, low-occurrence situations, Dreves says.
“The technology used in a simulation lab combines real clinical gear, robotic, full-body simulators, simulation-specific monitoring, wireless controllers, communication equipment and audiovisual recording apparatus,” says Todd Dadaleares, Southern Maine Community College’s healthcare simulation operations specialist. “At times, clinical actors or standardized patients will be trained to play specific roles as a patient, family member or embedded participant to guide the simulation and/or the learners through the scenario.”
He adds, “A well-run simulation should have all the elements of a well-rehearsed one-act play.”
Debrief
Simulation has numerous benefits. Unlike real life, instructors can stop and restart scenarios, giving students time to ask questions and practice maneuvers.
The quality and ease of use of today’s simulators has improved vastly, requiring hand-held computer tablets and monitors.
“There used to be a massive computer,” says McManus. “Our first simulator had a room that ran the compressor. All the wires and the compression hoses came through the wall and hooked to the mannequin.”
Also useful is the ability to record simulations, allowing for playback and constructive critique.
Dreves says simulation is used across the Southern Maine Community College nursing curriculum in various ways.
“In our beginning semesters, simulation is a great way to safely demonstrate assessments, medication administration, interventions such as intramuscular injections and urinary catheter insertions,” Dreves says.
In later semesters, high-fidelity mannequins can simulate scenarios such as childbirth and life-threatening scenarios across the lifespan, from infant to adult, to assess how students use the nursing process and clinical judgment to intervene.
The focus on simulation picked up during the pandemic, when certain clinical areas were no longer able to accommodate clinical experiences such as pediatrics, maternity and mental health areas, Dreves notes.
New equipment costs for high-tech full-body simulators can be $60,000 to $70,000, says Dadaleares. But there remains another barrier – not enough space to expand simulation capacity and, in turn, workforce development capacity.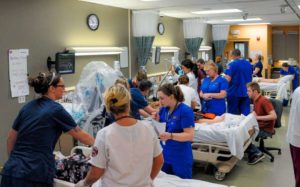
Building confidence
Dreves says studies show adult learners absorb and remember more information if it’s presented with an appropriate amount of stress and realism.
“Perhaps the student makes a mistake or the scenario was designed to progress to a decision that forces a difficult conversation or action,” she says.
Students who simulate learn more from their mistakes than from their successes. The lab provides a safe space to do so, building confidence.
“It gives students an opportunity to attain some level of comfort with more complicated intervention and assessment skills, so when they’re with a live patient in a real-world scenario, they have skills and the confidence that they know how to intervene appropriately,” says Erin Soucy, dean of undergraduate nursing at the University of Maine at Fort Kent.
The Fort Kent campus recently acquired a holographic obstetrics simulator, allowing students and instructor to don headsets to study fetal development.
Another benefit to simulation, Soucy says, is that people are able to practice “low-frequency but high-risk patient care situations.” For example, particularly in rural areas, a nurse might go years without seeing an obstetrical complication – but if one occurs, they need to know how to intervene immediately.
Realistic scenarios
In Wells, York County Community College partnered with Southern Maine Community College to implement new high-fidelity simulators for the York County campus’s Advanced Emergency Medical Technician program, funded through the Maine Jobs & Recovery plan and a Harold Alfond Foundation grant. (The training, including books and supplies, is free for Maine residents who meet the grant requirements.)
The money allowed the program to buy adult, child, and birthing mother and baby simulators, says Donald Sheets, co-chair of Southern Maine’s Emergency Medical Services Department. “We’re using those in our lab settings to create as realistic scenarios as we can,” Sheets says.
For example, students can check pulses, listen to lung sounds, and monitor cardiac rhythms. “We’re creating different scenarios where students can assess things on the simulator that we’d want them to check on a live patient,” he says.
Leah Mitchell, a former simulation instructor and currently the department’s co-chair, says simulators help provide students with experience to fulfill training requirements. “For our EMT students to graduate, they have to do 10 patient encounters,” Mitchell says.
Due to the pandemic and EMT workforce shortages, that number couldn’t be guaranteed through fieldwork in recent years. The simulators fill the gap. Sheets credits state funding for advancing education and workforce development.
“These simulators are very hard for us to ever budget for,” he says. “When grant funds come around, it gives us the opportunity to purchase new simulators that we wouldn’t otherwise be able to.”
There’s a world of difference between today’s simulators versus those in the past.
“You’re looking at a more realistic experience for all the senses,” says Mitchell. “Twenty years ago, you could do some airway management and some baseline cardiac monitoring. Now you can do surgical procedures.”
Virtual anatomy
Another educational tool is the virtual anatomy table. “Using this technology, we’re able to visualize complete anatomical systems in 3D and show how they work as a unit,” Northern Maine Community College biology instructor Trena Soucy has said. “The table brings anatomy to life and off the pages of a text book, increasing the students’ understanding of how the body works in parts and as a whole.”
The technology should never replace real-life clinical work, says McManus.
“But there are things students aren’t allowed to do in clinical real-life situations that they can do here,” McManus says. “For example, students aren’t allowed to give blood in the hospital. As a nurse, the first time you give blood is the first time you’ve done that procedure. But students can get that experience in our simulation lab. It allows us to teach skills that students can’t get as a student. It better prepares graduates for what they’ll face in the real world.”
She adds, “It’s a very exciting to be a student or a teacher in the health care professions.”
Specialized training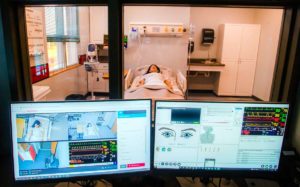
In 2021, Northern Maine Community College in Presque Isle secured a $1 million grant to develop a 5,000-square-foot emergency medical service simulation lab to allow year-round indoor training with the program’s ambulance, purchased in 2020, along with interactive mannequins and audio-visual technology to allow instructors to view and record scenarios.
The expansion reflects Aroostook County’s increasing need for paramedics and the resulting increased enrollment in the EMS technician and paramedic programs.
Since 2018, NMCC EMS students have had access to Trauma Hal, a lifelike training mannequin housed in the Nursing Simulation Center. The new space provides access to additional specialized simulators and training equipment.